Are you at risk for heart failure?
Learn about six factors—including excess weight and certain medications—that could raise your risk of this heart condition.
Updated on March 11, 2024

Can you lower your risk for heart failure? In a word: yes.
While some risk factors for this common heart condition, such as family history and congenital heart disease (heart problems that are present at birth), are out of your control, there are many lifestyle changes you can make to lower your risk. And since heart failure is usually caused by damage that weakens… Show More
Can you lower your risk for heart failure? In a word: yes.
While some risk factors for this common heart condition, such as family history and congenital heart disease (heart problems that are present at birth), are out of your control, there are many lifestyle changes you can make to lower your risk. And since heart failure is usually caused by damage that weakens the heart muscle, the same approaches can also help prevent a heart attack.
Maintaining a healthy lifestyle is “paramount,” says Andrew Behunin, DO, a cardiologist at MountainStar Heart Center at St. Mark’s Hospital, in Salt Lake City, Utah. In his experience, being active and mindful of your food choices are among the most effective ways to improve your heart health.
Keep reading to learn more about risk factors for heart failure, and what you can do to lower each of them.
Show Less
High blood pressure
Arteries are the pipelines that carry blood from your heart to other parts of your body. Systolic blood pressure measures the force of your blood flowing through your arteries when your heart beats. Diastolic blood pressure measures this force when your heart relaxes. In a blood pressure reading,… Show More
Arteries are the pipelines that carry blood from your heart to other parts of your body. Systolic blood pressure measures the force of your blood flowing through your arteries when your heart beats. Diastolic blood pressure measures this force when your heart relaxes. In a blood pressure reading, systolic blood pressure is the top number and diastolic is the bottom.
Having high blood pressure—also called hypertension—means your heart has to work harder to pump blood, which over time can weaken and stiffen the muscle. It also contributes to hardening of the arteries, leading to decreased blood flow to your heart. People with high blood pressure have a higher risk of stroke, heart failure, and heart attack.
Lower your risk: Some people may not even know they have high blood pressure. It’s important for adults to be screened at least every year by a healthcare provider (HCP). In some cases, your HCP may want to measure your blood pressure more frequently.
If you’ve been diagnosed with high blood pressure, talk to your HCP about treatment options. It’s important to make lifestyle changes that include managing weight, limiting salt, eating a well-balanced diet rich in fruits and vegetables, reducing alcohol intake, quitting smoking, and staying physically active as you are able. All of these will go a long way toward keeping your blood pressure in the healthy range. Your HCP may suggest the use of medications, as well.
Show Less
Obesity
Excess weight can raise blood pressure and blood cholesterol (a type of fat in the blood). It can also lower HDL (“good” cholesterol) and strain the heart.
Lower your risk: Losing about 2.2 pounds of body weight can potentially lower your blood pressure by one point. To lose weight, try these… Show More
Excess weight can raise blood pressure and blood cholesterol (a type of fat in the blood). It can also lower HDL (“good” cholesterol) and strain the heart.
Lower your risk: Losing about 2.2 pounds of body weight can potentially lower your blood pressure by one point. To lose weight, try these strategies:
- Set a series of realistic short-term goals to help you reach your long-term goal.
- Keep a food diary to track how much you eat, aiming to reduce your daily calorie intake.
- Combine a healthy diet rich in fruits and vegetables and low in salt and saturated fat (fat that is solid at room temperature) with exercise. As you are able, try to log at least 150 minutes of moderate-intensity physical activity per week—brisk walking, for instance. Work with your HCP to figure out the best type of exercise for you.
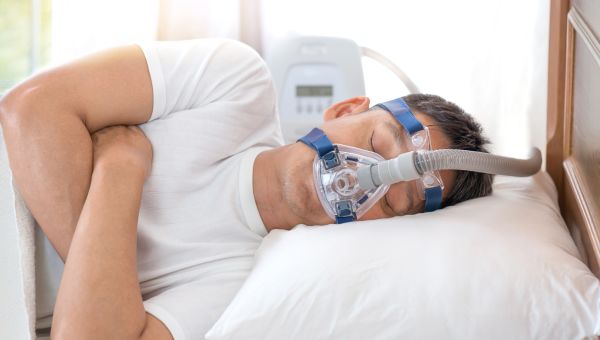
Sleep apnea
When you have this common sleep disorder, your upper airway is repeatedly blocked during sleep, reducing or completely stopping airflow. This could cause pauses in breathing that affect your health over time. The National Institutes of Health has reported that people with sleep apnea may be at an… Show More
When you have this common sleep disorder, your upper airway is repeatedly blocked during sleep, reducing or completely stopping airflow. This could cause pauses in breathing that affect your health over time. The National Institutes of Health has reported that people with sleep apnea may be at an increased risk for heart disease. Left undiagnosed or untreated, the condition can lead to serious complications, including heart failure or a heart attack.
Lower your risk: For most people with heart failure and sleep apnea, treatment generally involves a combination of losing weight and using a continuous positive airway pressure (CPAP) machine while you sleep. A CPAP machine keeps your airways open by delivering mild pressure through a mask that you wear on your face while you sleep. Following a heart-healthy diet rich in fruits and vegetables and low in salt and saturated fat (which is solid at room temperature), as well as getting regular exercise as you are able can be the first steps you take toward weight loss. Treating sleep apnea can also improve your blood pressure, a risk factor in developing heart failure.
Show Less
Smoking
While you already know that smoking is bad for your health, you may not know how it damages your heart. If you smoke a cigarette, you’re temporarily increasing your heart rate and blood pressure. Smoking contributes to hardening of your arteries and damages heart muscle tissue directly.
No matter… Show More
While you already know that smoking is bad for your health, you may not know how it damages your heart. If you smoke a cigarette, you’re temporarily increasing your heart rate and blood pressure. Smoking contributes to hardening of your arteries and damages heart muscle tissue directly.
No matter how many years you’ve been smoking, there are plenty of benefits to quitting right now. Once you stop smoking, heart health immediately improves and you start to reduce your risk for heart disease. Even people who have already had a heart attack can cut their risk of another once they quit.
Lower your risk: If you’re unable to quit smoking on your own, talk to your HCP about available tools. Research suggests that behavioral support—whether it’s face-to-face, via phone call, or online—and using quit aids, like patches, lozenges, gum, or prescription drugs, can be effective treatment.
“There are lots of quit aids, but ultimately there’s no magic bullet,” says Behunin. “What it requires is having a personalized plan—whether it’s quitting abruptly or with the help of nicotine gum or prescription medications—and someone like a quit coach who will hold you accountable.”
Show Less
Certain medications
If you have risk factors for heart failure, it’s important to talk to your HCP about any medications you take. Some medications may lead to complications including nonsteroidal anti-inflammatory drugs (NSAIDs). Over-the-counter NSAIDs (like ibuprofen and naproxen) and prescription varieties can… Show More
If you have risk factors for heart failure, it’s important to talk to your HCP about any medications you take. Some medications may lead to complications including nonsteroidal anti-inflammatory drugs (NSAIDs). Over-the-counter NSAIDs (like ibuprofen and naproxen) and prescription varieties can worsen the risk for heart failure for people with underlying heart and blood vessel issues.
Lower your risk: Make sure everyone on your healthcare team has a full list of the medications you’re taking. Ask your HCP about potential interactions, or if a medication could increase your risk of a heart problems. They can tell you whether the benefits of continuing to take a drug outweigh the risks associated with it.
Show Less
Drinking alcohol
Heavy drinking over a long period of time can increase your risk for heart failure, and lead to alcoholic cardiomyopathy, a form of heart disease. Even those who drink in moderation should discuss the risks with their HCP.
Lower your risk: If you drink, do so in moderation only after consulting… Show More
Heavy drinking over a long period of time can increase your risk for heart failure, and lead to alcoholic cardiomyopathy, a form of heart disease. Even those who drink in moderation should discuss the risks with their HCP.
Lower your risk: If you drink, do so in moderation only after consulting your HCP. According to the government's 2020-2025 Dietary Guidelines for Americans, that means no more than two drinks per day for men and one drink per day for women. Remember: A drink is a 12-ounce beer, a 4-ounce glass of wine, 1 1/2 ounces of 80-proof liquor or 1 ounce of 100-proof liquor. If you don’t drink, there is no health benefit to starting.
Show Less
National Heart, Lung, and Blood Institute. Heart failure treatment. Page last updated March 24, 2022.
National Heart, Lung, and Blood Institute. What is heart failure? Page last updated March 24, 2022.
Centers for Disease Control and Prevention. Heart Failure. Page last reviewed January 5, 2023.
National Heart, Lung, and Blood Institute. What is high blood pressure? Page last updated March 24, 2022.
Centers for Disease Control and Prevention. High blood pressure symptoms and causes. Page last reviewed May 18, 2021.
Centers for Disease Control and Prevention. Know your risk for high cholesterol. Page last reviewed March 20, 2023.
Centers for Disease Control and Prevention. Losing weight: Getting started. Page last reviewed June 3, 2022.
Centers for Disease Control and Prevention. Physical activity for a healthy weight. Page last reviewed June 16, 2022.
Neter JE, Stam BE, Kok FJ, et al. Influence of weight reduction on blood pressure: a meta-analysis of randomized controlled trials. Hypertension. 2003 Nov;42(5):878-84.
National Institute of Neurological Disorders and Stroke. Sleep Apnea. Page last reviewed January 20, 2023.
National Heart, Lung, and Blood Institute. Benefits of quitting smoking. Page last updated March 24, 2022.
Johns Hopkins Medicine. Smoking and cardiovascular disease. Accessed on March 25, 2023.
Centers for Disease Control and Prevention. How to quit. Page last reviewed June 17, 2021.
UpToDate. NSAIDs: Adverse cardiovascular effects. Page last updated February 2022.
Johns Hopkins Medicine. Alcohol and heart health: Separating fact from fiction. Accessed on March 25, 2023.
US Department of Food and Agriculture. Dietary Guidelines for Americans, 2020-2025 – Make every bite count with the dietary guidelines. Accessed on March 25, 2023.
More On


video

article

slideshow


video


video
