Acne
- What is acne?
- What are the types and symptoms of acne?
- What causes acne?
- What are the risk factors for developing acne?
- How is acne diagnosed?
- When should I see my healthcare provider?
- How is acne treated?
- What are the complications of acne?
- Can you prevent acne?
- What is the outlook for acne?
- Living with acne
- Featured acne articles
Introduction
Acne (also called acne vulgaris) is the most common skin condition in the United States. It affects more than 80 percent of people in the U.S. at some point in their lives. The condition occurs when pores become clogged with dead skin cells and oil. (Pores are tiny holes in the skin that allow oil and sweat to move from glands under the skin to the skin’s surface.) Acne commonly appears as whiteheads, blackheads, and pimples. With treatment, most cases of acne can be reversed or improved.
Get the facts about acne, including why it happens, what it looks like, and what acne medications can treat stubborn breakouts. Learn what steps you can take to achieve clearer skin at home and how you may be able to prevent acne from appearing at all.
What is acne?

Acne refers to several types of blemishes or spots that can occur on the skin of your face, chest, shoulders, or back. It often develops in children and teenagers who are experiencing puberty (the period when young people reach sexual maturity). For many people, acne naturally resolves in early adulthood, though this isn’t always the case.
People assigned female at birth (AFAB) are more likely to have acne in adulthood than people assigned male at birth (AMAB). According to the American Academy of Dermatology Association, around 20 to 40 percent of people AFAB with adult acne experience it for the first time as an adult.
In general, acne is caused by a buildup of dead skin cells and sebum. Sebum is an oily substance naturally produced by the body that helps keep skin moisturized. It’s made by tiny organs under the skin called sebaceous glands.
This buildup occurs in pores, the small openings in the skin that contain hair follicles and secrete sebum. Hair follicles are structures that grow hair. The follicles are lined with a type of skin cell called keratinocytes.
The body continually sheds skin and grows new skin cells. As this happens, keratinocytes and sebum rise to the surface of the skin through pores. Acne occurs when sebum, keratinocytes, and hair become trapped in pores. Bacteria that naturally lives on the skin’s surface may also grow in a clogged pore, which can lead to inflammatory acne (see more below).
What are the types and symptoms of acne?

Acne vulgaris, the most common type of acne, has several forms. The main forms of acne include:
- Blackheads: These are clogged pores that open on the surface of the skin. The black part of a blackhead isn’t dirt. Instead, a chemical reaction causes sebum to turn dark when it’s exposed to oxygen in the air.
- Whiteheads: These are white or flesh-colored bumps that occur when dead skin cells and sebum collect in pores but don’t break the surface of the skin. Along with blackheads, whiteheads are sometimes called comedones (or sebaceous plugs in pores).
- Papules: These are small, inflamed bumps that are usually tender to the touch and may be red or a few shades darker than your skin tone.
- Pimples: Also called pustules or zits, pimples are papules that contain pus (a thick, white or yellow fluid made of dead cells). The base of a pimple may be red or discolored.
- Acne nodules: These are large, painful bumps that feel solid. They may be swollen, discolored, and tender to the touch. Nodules can occur when dead skin cells, oil, and bacteria become trapped underneath the skin.
- Cystic acne (or cysts): These are acne nodules that become filled with pus. They’re rooted underneath the skin and are often painful and tender to the touch. Because they contain pus, they’re softer than firm nodules.
Acne may also be labeled according to its cause. For example, hormonal acne is often related to the hormonal changes that occur during puberty and menstruation. Fungal acne occurs when yeast (a type of fungi) accumulates in and blocks pores. Pomade acne refers to breakouts on the forehead that are caused by oily hair products.
Inflammatory vs. non-inflammatory acne
Inflammation is one of the body’s primary ways of eliminating threats to your health. If acne causes the wall of a pore to break down, the contents (sebum, dead skin cells, and bacteria) can empty into nearby tissue. Your body sees this as a threat and triggers inflammation to neutralize the problem.
Inflammatory acne typically appears red or discolored, swollen, and painful. It often contains pus. Types of inflammatory acne include papules, pimples, nodules, and cysts.
Non-inflammatory acne doesn’t involve inflammation. Whiteheads and blackheads are examples of non-inflammatory acne.
What causes acne?

Acne can occur if a pore gets filled with:
- Dead skin cells
- Excess sebum
- Bacteria
Your face alone has thousands of pores, so the occasional pimple or blackhead is bound to happen. Still, some lifestyle factors can play a role in triggering or worsening acne. These include:
- Not getting enough sleep
- Wearing snug-fitting clothes, hats, helmets, backpacks, or sports equipment that can irritate the skin or not allow it to breathe
- Exfoliating or scrubbing your skin too hard
- Smoking
- Exposure to environmental irritants, including humidity and pollution
- Picking at or squeezing skin blemishes
- Using oil-based skincare or hair care products
- Stress, which can increase hormone levels and sebum production
- Taking certain medications, including but not limited to isoniazid (an antibiotic), lithium (used to treat certain mental health conditions), phenytoin (an anticonvulsant), and certain medications that affect hormones, such as steroids and some forms of birth control.
- Eating certain foods
Experts are still learning how diet influences skin health. Research suggests that drinking cow’s milk may lead to acne, though there’s no evidence that cheese or yogurt made with cow’s milk causes acne.
Other products with possible links to acne include whey protein, carbohydrate-rich foods like bagels and chips, sugary beverages, and items that are high in both fat and sugar (such as doughnuts and milkshakes). Many acne-triggering foods have a high glycemic index, which means they can sharply increase blood sugar levels.
What doesn’t cause acne
There are a number of common misconceptions around the causes of acne. Despite popular belief, there’s little evidence that any of the following can cause a breakout:
- Eating chocolate, especially dark chocolate (that said, frequently consuming sugary foods or drinks may contribute to acne)
- Masturbating or having sex
- Having dirt on your skin
- Wearing makeup (although oil-free cosmetics are best if you want to avoid acne)
What are the risk factors for developing acne?

Most people experience acne at one point or another. But certain acne risk factors may leave you more prone to prolonged or severe breakouts. These include:
- Age: Levels of male hormones called androgens increase in both people AMAB and AFAB during puberty. Androgens cause sebaceous glands to grow and produce excess sebum, potentially leading to acne.
- Hormones: In addition to the hormonal changes that occur during puberty and periods of stress, a person AFAB can experience acne-causing changes in hormones during pregnancy or before, during, or after their menstrual period.
- Family history: You may be more likely to experience severe acne if a parent or another close blood relative had or has it.
How is acne diagnosed?
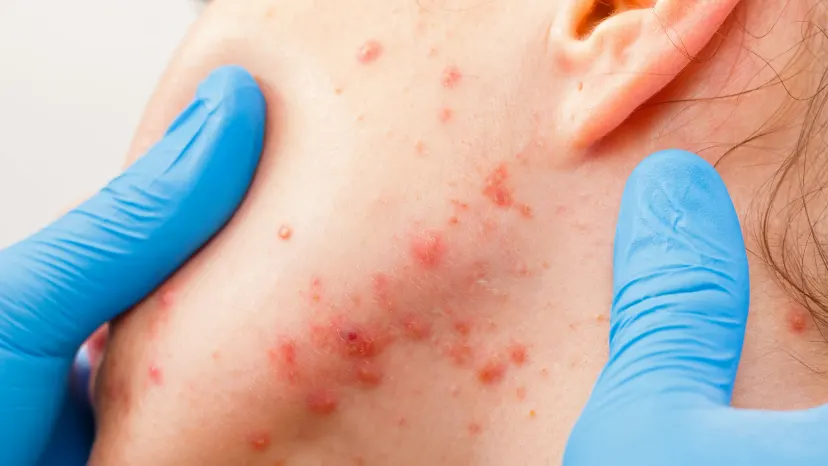
Diagnosing acne is relatively straightforward. Your HCP will examine your skin and ask you a series of questions. You may discuss:
- How long you’ve had skin blemishes and where on your body they tend to occur
- If you’re experiencing any other symptoms
- How certain activities or events (such as menstrual periods) affect your complexion
- Your stress levels, eating habits, and sleep patterns
- Any medications or supplements you’re taking (or recently stopped taking)
- Your family medical history, including if a close blood relative (such as a parent or sibling) has acne or previously had it
Your HCP might run tests to rule out possible medical causes of acne, especially if you’re an adult with severe acne that occurred suddenly. Although uncommon, acne may be a sign of hormonal conditions like polycystic ovary syndrome, Cushing’s syndrome, and insulin resistance. Sudden acne could even indicate pregnancy. Sometimes, more complex skin conditions like perioral dermatitis (an inflammatory condition that involves a rash around the mouth) and hidradenitis suppurativa are mistaken for everyday acne.
When should I see my healthcare provider?

It’s never too early to speak with a healthcare provider (HCP) about acne. Even if your breakouts are mild, your primary HCP or a dermatologist can examine your skin and suggest ways to enhance your complexion. Early intervention can help prevent acne from worsening and causing complications like scarring.
It’s also important to speak with an HCP if:
- Your acne is persistent or becomes severe
- You’re an adult and your acne occurs suddenly
- An over-the-counter (OTC) or prescription acne treatment worsens your acne or causes skin irritation
Although rare, some skincare products can trigger severe allergic reactions. Call 911 or seek immediate care at a hospital emergency department (ED) if any of the following occur after using a skincare product:
- Trouble breathing
- Weakness or loss of consciousness
- Throat tightness
- Swelling of the face, tongue, lips, or eyelids
What questions should I ask my healthcare provider?
Don’t hesitate to ask your HCP questions about your acne and how you can improve your skin health. Some basic questions you may want to ask about acne and its treatment include:
- What type of acne do I have?
- Should I speak with a dermatologist? If so, can you refer me to a specialist you recommend?
- What OTC treatments could improve my acne?
- What self-care measures could improve my acne? Should I avoid certain activities?
- Should I change my diet?
- What lotions, soaps, or skincare products should I avoid? What should I try?
- Do I need prescription acne treatment? If so, what treatments do you recommend?
- When should I expect to see improvement in my acne?
- What are the possible side effects of acne medication?
- Is it safe to stop using acne medication if it doesn’t work?
- When should I contact you? Is there a scenario in which I should seek emergency care?
How is acne treated?

Acne may be treated by your primary HCP or a dermatologist. Your HCP will consider several factors when creating an acne treatment plan, including:
- Your age and sex assigned at birth
- What type of acne you have
- The location of your acne
- When your acne started
- What acne treatments you’ve already tried
- If you have acne-related dark spots or scarring
Based on your needs, your HCP may recommend one or more of the following acne treatment approaches:
Topical medications
Topical medications are creams, soaps, gels, lotions, or pads that you apply to your skin. There are several types of topical acne medications, which include but are not limited to:
- Benzoyl peroxide: Found in many OTC acne products, benzoyl peroxide works by eliminating bacteria and helping to decrease sebum production.
- Salicylic acid: OTC topical treatments containing salicylic acid are often used to help break down blackheads and whiteheads and prevent hair follicles from becoming blocked.
- Topical retinoids: Derived from vitamin A, retinoids and retinoid-like drugs can clear and prevent acne, reduce skin inflammation, and improve acne scarring. Examples of topical retinoids include adapalene, tretinoin, and tazarotene. These products increase sensitivity to the sun as a side effect and can cause skin irritation and dryness, so start slow. Your HCP may recommend applying a retinoid a few nights a week and gradually working your way up to daily use.
- Topical antibiotics: Antibiotics (such as clindamycin and erythromycin) in gel or cream form may be prescribed to reduce excess skin bacteria and ease inflammation. These topical medications are often combined with benzoyl peroxide or retinoids.
- Azelaic acid: Azelaic acid offers antibiotic properties that can help address acne and skin discoloration when used as directed. Prescription products with azelaic acid may be an option for people who are pregnant or breastfeeding.
- Dapsone: This prescription gel is often recommended for people AFAB with inflammatory acne.
Skin irritation, dryness, burning, or discoloration may occur with topical acne treatments. Speak with your HCP if you experience any unexpected side effects.
Oral medications
Some people with moderate to severe acne experience positive results with oral acne medications. These are treatments that you take in pill form. Depending on your needs, your HCP may prescribe:
- Isotretinoin: This oral retinoid helps open pores, which allows topical medications to more effectively penetrate skin and treat acne. Isotretinoin itself can also help clear breakouts and minimize acne scarring.
- Oral antibiotics: Antibiotics in pill form may be prescribed to treat more severe breakouts, such as nodular acne. Oral antibiotics can help stop bacteria growth on skin and ease inflammation.
- Oral contraceptives: In addition to preventing pregnancy, some oral contraceptives (birth control pills) that contain the hormones estrogen and progestin can help clear acne in people AFAB. It may take a few months for results to appear.
- Oral corticosteroids: Taking corticosteroids (such as prednisone) can help reduce inflammation in people with severe nodular acne and other difficult-to-treat inflammatory breakouts.
- Anti-androgen agents: An anti-androgen drug called spironolactone can help prevent androgen hormones from increasing oily sebum production and causing acne. This is usually recommended for people AFAB who don’t experience improvement with oral antibiotics.
As is the case with most medications, oral acne treatments come with the potential for side effects. Your HCP can outline the possible risks of taking acne medication and help you make confident decisions about your treatment.
For example, taking isotretinoin when pregnant can cause severe harm to a developing fetus. Pregnant people and those who are breastfeeding should never take isotretinoin and people AFAB who are prescribed isotretinoin are often advised to take birth control to prevent pregnancy.
Never stop taking an acne medication or adjust your dosage without first speaking with your HCP.
Therapies and procedures
Not every case of acne can be resolved with topical or oral medications. Some people with persistent or severe forms of acne may respond well to additional therapies and procedures, such as:
- Chemical peels: A superficial chemical peel involves repeatedly applying a solution of acne-reducing chemicals (such as salicylic acid) onto the skin to remove old skin cells. Over time, chemical peels can improve your skin’s appearance and texture. Your HCP may be able to perform chemical peels or recommend an OTC product.
- Light therapy: Light-based acne treatments such as infrared light therapy and photodynamic therapy can help some people improve their complexion. Results can be mixed, though. Your HCP can determine if you’re a possible candidate for light therapy.
- Corticosteroid injection: Injecting a corticosteroid (such as triamcinolone) directly into the affected area of skin can help clear breakouts and quickly relieve pain associated with deep, inflamed nodular or cystic acne. Receiving this treatment more than a few times, however, can cause side effects like skin thinning and discoloration.
- Extraction: Your HCP may use special instruments to carefully express (squeeze) and remove pimples, whiteheads, blackheads, and cysts one by one.
Diet changes
Research suggests that changing your diet may improve your complexion and help treat acne. While high-glycemic foods (foods that raise your blood sugar levels) are staples in the average American diet, some studies show that consuming more low-glycemic foods can help clear acne breakouts.
Examples of low-glycemic foods include:
- Green vegetables
- Some fruits, including cherries, peaches, apples, pears, berries, grapefruit, and apricots
- Legumes, including lentils, chickpeas (garbanzo beans), and kidney beans
- Nuts
- Brown rice
- Whole grain breads and pastas
- Steel-cut oats
On the other hand, high-glycemic foods that may contribute to acne include:
- White breads and pastas
- White rice
- Bagels
- White potatoes and products made from potatoes, including chips and fries
- Crackers
- Many packaged breakfast cereals
- Doughnuts, croissants, cakes, and many commercially baked goods
If you suspect that your diet is exacerbating your acne, think about what foods or beverages seem to cause or worsen your breakouts. Try eliminating this food or beverage for a few days, weeks, or a month and see how your skin responds.
Treating acne at home
Practicing good skincare habits at home is an essential part of effective acne treatment. To help set your skin up for success, be sure to:
- Use a gentle skin cleanser. Avoid harsh soaps, toners, and scrubs, including products that contain alcohol. Wash your face twice daily with warm (but not hot) water, especially after exercising or working up a sweat.
- Remove makeup before going to bed. If you wear makeup, opt for oil-free products that won’t clog pores. These may be labeled as non-comedogenic or non-acnegenic.
- Wash your hair regularly. This is particularly important if your hair is naturally oily. Having greasy hair or using oil-based hair products can cause or worsen acne on your temples or forehead (a common issue called “pomade acne”).
- Moisturize. Use an oil-free moisturizer as directed to avoid dry skin, which can make acne worse by causing dead skin cells to accumulate.
- Shave wisely. Be sure to use a sharp blade and prep your skin with water and soap before applying shaving cream. Be slow and gentle when shaving, and don’t shave more often than you need to.
- Protect your skin. Wear an oil-free sunscreen and avoid spending too much time in the sun. Many acne treatments can make you more prone to sunburns and melasma (a type of skin discoloration that may be triggered by sun exposure).
- Take a hands-off approach. As tempting as it may be to squeeze pimples or pick at breakouts with your fingers, it’s best to avoid touching your face. It can exacerbate acne and lead to complications like scarring.
These are general tips for treating acne at home. For personalized skincare advice, speak with your HCP.
What are the complications of acne?

Promptly treating acne after it develops can help prevent complications. The two main complications of acne are scarring and discoloration:
Acne scarring
Acne scarring refers to long-lasting skin irregularities that occur once acne heals. An acne scar can be raised or create a slight indent in your skin. Your skin may appear pitted (similar to the texture of an orange peel), or you may develop a thick raised scar, known as a keloid.
Factors that increase your risk of acne scarring include:
- Being a person of color or having a darker skin tone
- Having one or more first-degree relatives with acne scarring
- Experiencing acne for a long period of time, either because it was left untreated or because treatment was ineffective
Treatment for acne scars will depend on the type and severity of scarring. Some people experience positive results after trying chemical peels or topical treatments like retinoids. Injectable fillers can be used to plump up scarred areas of skin that appear “sunk in.” In other cases, minor surgical procedures may be recommended to remove raised acne scars.
These aren’t all the possible treatments for acne scarring. Speak with your HCP to learn what options may be best for you.
Skin discoloration
Acne that clears may leave behind a flat, discolored mark on your skin. This mark may be darker than your general skin tone (known as hyperpigmentation) or lighter than your general skin tone (hypopigmentation). Most cases involve areas of darkened skin, which is known as post-inflammatory hyperpigmentation.
People of color and those with darker skin tones are more likely to develop skin discoloration after acne since their skin contains additional melanin (a substance that produces skin pigment). Still, this acne complication is relatively common and can affect anyone.
In general, skin discoloration is easier to treat than acne scarring. Many people can address discoloration by using topical treatments containing a retinoid, azelaic acid, or hydroquinone (a skin-lightening agent). Other possible treatment options include products with glycolic acid, vitamin C, or kojic acid. Your HCP can help you select the ideal treatment regimen for your needs.
Can you prevent acne?

It’s not always possible to prevent acne. This is especially true if you’re going through hormonal changes that occur during puberty, pregnancy, or menstruation. You may also be naturally prone to breakouts if you have a family history of acne.
Regardless of your likelihood of getting acne, there are steps you can take to reduce your risk
and minimize the severity of breakouts if they do occur:
- Wash your skin daily with a gentle cleanser and warm water. Avoid washing too frequently or vigorously scrubbing your skin. It’s particularly important to clean your skin if you’re sweaty from exercise or being outdoors.
- Resist the urge to touch your face. This can help reduce the spread of oil and bacteria on your skin.
- Avoid wearing tight-fitting clothes if you’re prone to acne on your chest, shoulders, or back.
- Choose oil-free skincare products and cosmetics. These may be labeled as non-comedogenic or non-acnegenic. Remember to wash your face before going to bed if you wear makeup. It’s also wise to use an oil-free moisturizer to prevent dry skin.
- Use water-based hairspray and styling creams and gels instead of oil-based products that can cause pomade acne.
What is the outlook for acne?

Acne resolves on its own for some people in early adulthood. Overall, the outlook for acne vulgaris is generally positive with appropriate treatment. Most people can reverse acne and improve their skin, though it may take some time to find the right combination of routine skincare and acne treatments. There’s no one-size-fits-all treatment for acne. What works for someone else may not work for you.
Acne scars and skin discoloration are sometimes more challenging to treat than the acne itself. Even so, many people can enhance their skin’s appearance with treatment. Consider speaking with a dermatologist if you’re dealing with stubborn acne or acne complications.
Living with acne

Whether you’ve had acne for years or skin blemishes are a new issue for you, acne can be upsetting and unpredictable. Thankfully, effective treatment options exist. Partnering with an HCP for acne treatment and staying consistent with your skincare routine can improve your skin.
To ensure you achieve the best results, it’s important to attend all scheduled medical appointments and continue to follow your acne treatment plan—even when your acne appears to be healed. Your HCP may adjust your treatment to focus on maintaining your results and helping you avoid breakouts in the future.
Acne and mental health
Acne isn’t a life-threatening issue, but the effects of this skin condition can still take a toll on your mental health. It’s common for acne to negatively affect self-esteem, self-image, and quality of life. Some people with acne feel embarrassed or hesitant to leave their home or attend social events. Others may experience symptoms of anxiety or depression. The emotional issues related to acne can cause stress, which can in turn make acne worse.
There’s no universal way to cope with acne and the emotions it can produce. Still, it’s important to remember that acne is remarkably common and treatable. In most cases, the appearance of acne is outside your control and very little to do with your lifestyle or habits. Having acne is not your fault and it doesn’t mean you are unclean or unhealthy.
That said, as you work with your HCP to find effective acne treatment, it can be helpful to practice general healthy habits to boost your overall wellness. That could include steps like these:
- Keep doing your favorite hobbies and activities, whether they are painting, cooking, playing music, or watching classic movies.
- Stay connected with friends and family. Don’t isolate yourself because of acne.
- Work on managing stress with time-tested techniques like yoga, meditation, deep breathing, and journaling.
- Prioritize your overall health by getting enough sleep, exercising regularly, and enjoying a well-balanced diet.
- Avoid drinking alcohol in excess, smoking, or using recreational drugs.
- Consult with a licensed mental health provider about your emotions and how you can navigate your thoughts in a healthy way.
Acne—and the negative emotions it can bring about—are issues that can be solved. Speak with an HCP to learn more about acne, its causes, and what treatment options can help you look and feel your best.
Featured acne articles

American Academy of Dermatology Association. Acne: Signs and Symptoms. Accessed February 14, 2024.
American Academy of Dermatology Association. Acne: Who Gets and Causes. Accessed February 14, 2024.
American Academy of Dermatology Association. Adult Acne. Accessed February 27, 2024.
American Academy of Dermatology Association. Acne Can Affect More Than Your Skin. Accessed February 27, 2023.
American Academy of Dermatology Association. Acne Scars: Consultation and Treatment. Accessed February 26, 2024
American Academy of Dermatology Association. Can the Right Diet Get Rid of Acne? Accessed February 15, 2024.
Cleveland Clinic. Acne. Last reviewed January 4, 2023.
Cleveland Clinic. Inflammatory Acne. Last reviewed April 19, 2022.
Harvard Health Publishing. A Good Guide to Carbs: The Glycemic Index. Published April 14, 2023.
Keri J. Acne Vulgaris. Merck Manual Professional Version. Last reviewed September 2022.
Mayo Clinic. Acne. Last reviewed October 8, 2022.
Meixiong J, Ricco C, Vasavda C, Ho BK. Diet and acne: A systematic review. JAAD Int. 2022;7:95-112. Published 2022 Mar 29.
National Institute of Arthritis and Musculoskeletal and Skin Diseases. Acne. Last reviewed July 2023.
Nemours TeensHealth. What Can I Do About Acne? Last reviewed August 2020.
Penso L, Touvier M, Deschasaux M, et al. Association between adult acne and dietary behaviors: Findings from the NutriNet-Santé Prospective Cohort Study. JAMA Dermatol. 2020;156(8):854-862.
Sangha AM. Managing post-inflammatory hyperpigmentation in patients with acne. J Clin Aesthet Dermatol. 2021;14(6 Suppl 1):S24-S26.
Skroza N, Tolino E, Mambrin A, et al. Adult Acne Versus Adolescent Acne: A Retrospective Study of 1,167 Patients. J Clin Aesthet Dermatol.
Sutaria AH, Masood S, Saleh HM, et al. Acne Vulgaris. StatPearls [Internet]. Last updated August 17, 2023.





